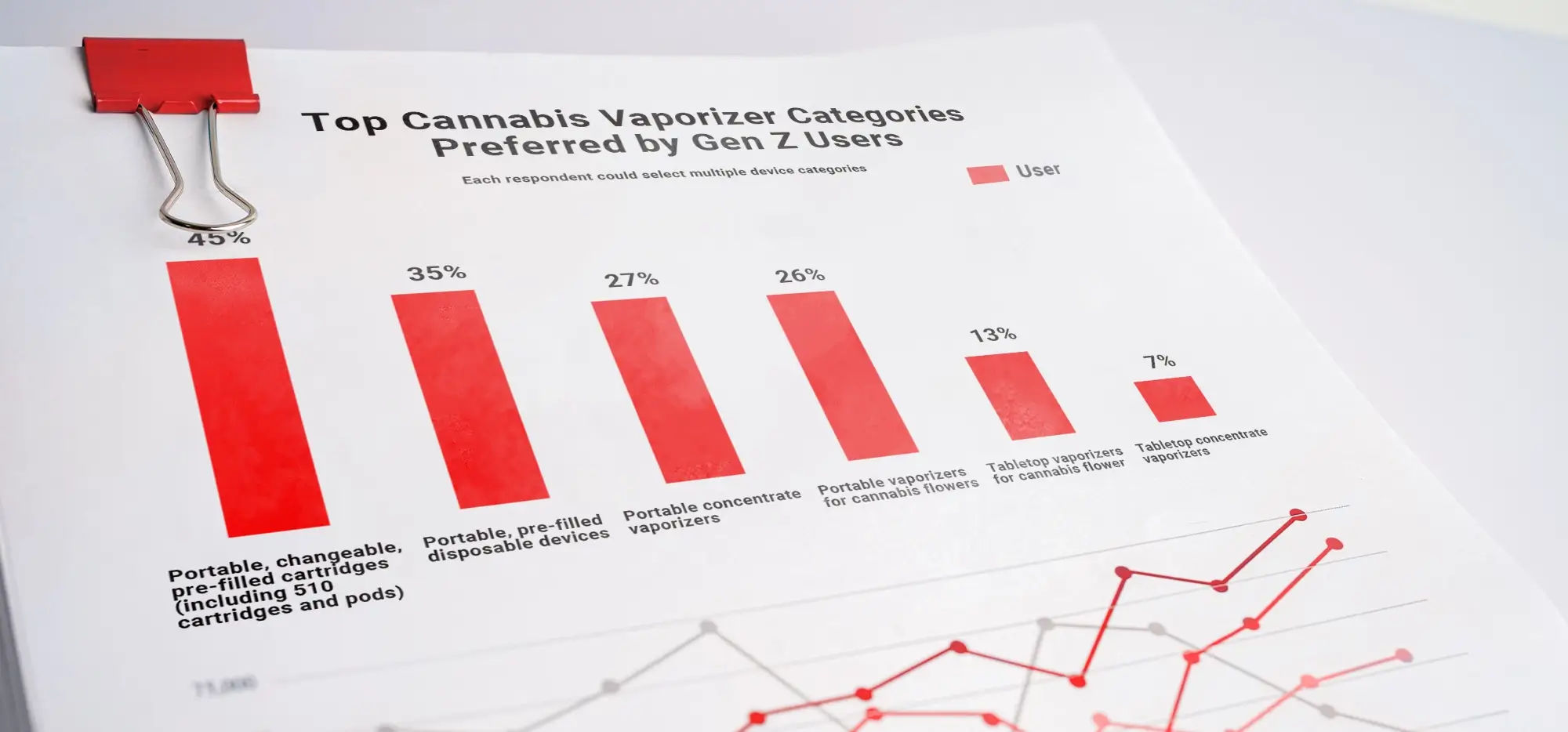
How to Sober Up from Weed Fast?
Last Updated: March 26, 2026
If you are searching how to sober from weed fast because you feel too high right now, the immediate goal is not detox. It is emergency grounding. Stop consuming, sit or lie down, cool your face, breathe out slowly, get to a quiet place, and remind yourself that panic, a racing heart, and distorted time are common with cannabis intoxication. If someone has chest pain, trouble breathing, a seizure, collapses, or cannot be awakened, seek emergency help immediately.
[Core Toolkit] 2026 Personal “Landing” Priority Matrix
| Target Demographic | Core Risk | Best First-Aid Tool | Physical Action Recommendations |
|---|---|---|---|
| Panicked newbie | Fear spiral, hyperventilation, racing heart | Reassurance plus slow exhale breathing | Sit down, cool face, breathe in for 4 and out for 6 to 8 |
| Edible overconsumer | Delayed peak, long duration, dose stacking | Time plus low-stimulation environment | No redosing, dim lights, sip water, lie down and wait it out |
| Older adult or medical user | Dizziness, blood pressure drop, fall risk | Lie flat and monitor | Raise legs if lightheaded, stand only with help |
| Person in a crowded setting | Sensory overload and social panic | Environmental withdrawal | Move somewhere dim and quiet, stay with one trusted person |
| Companion helping someone else | Missing a true emergency | Red-flag screening | Call emergency services for breathing trouble, collapse, seizure, or unresponsiveness |
Phase One: Physiological Control — Slow the Body First
When someone greens out, the body often panics before the mind does. The heart feels too fast, breathing gets shallow, and every sensation starts to feel dangerous. That is why the first response should be physical and simple, not complicated.
1. Splash Cold Water on the Face
Cooling the face can help interrupt a panic loop because facial cold stimulation is linked to the diving reflex, which can increase vagal influence and slow heart rate. In real use, that means a cold splash or cool washcloth can make the body feel less “stuck on high alert.” Do it while seated if the person is dizzy.
2. Use Slow Breathing With a Longer Exhale
Slow breathing does not remove THC, but it can reduce the intensity of the panic response. Reviews of slow breathing show effects consistent with increased parasympathetic activity and improved vagal regulation. A practical emergency pattern is inhale for 4 seconds and exhale for 6 to 8 seconds for 10 rounds. The key is not perfection. The key is making the exhale longer than the inhale.

Phase Two: Precision Intervention — Rescue by User Profile
The fastest relief comes from matching the response to the actual problem. Some users need reassurance. Some need to prepare for a long edible ride. Some mainly need fall prevention. Treating all of them the same wastes precious calm.
1. The Panicked Newbie: Reassure First, Explain Second
For the panicked beginner, the best first sentence is: “You took THC. This feels scary, but panic and paranoia are known effects, and most cases improve with reassurance and supportive care”. That matters because the fear of dying is often being fueled by normal intoxication symptoms such as a racing heart, dry mouth, derealization, and time distortion.
A more technical reassurance point can help some readers: cannabis does not usually cause the classic opioid-style fatal respiratory depression pattern, and cannabinoid receptor levels are relatively low in the medullary respiratory centers compared with opioid pathways. Still, if breathing is genuinely labored or the person becomes hard to wake, treat it as an emergency.
2. The “Edible” Victim: Accept the Timeline and Stop Redosing
Edibles cause some of the worst green-outs because they are delayed and deceptive. The CDC notes that edibles can take 30 minutes to 2 hours to produce effects, which leads many people to take more before the first dose peaks. The right move is to stop chasing a fix, lower the stimulation in the room, and plan for several hours of management rather than several minutes.
Oral THC also produces more 11-hydroxy-THC through liver metabolism, which helps explain why edible intoxication can feel stronger and last longer than inhaled cannabis. For this profile, the emergency intervention is environmental: lie down, dim lights, keep one calm person nearby, and do not take more THC.
3. Physically Sensitive Seniors / Medical Users: Prevent the Fall
For older adults or medically sensitive users, the danger may be dizziness more than panic. THC can increase heart rate and can contribute to orthostatic hypotension, meaning symptoms can worsen after standing up quickly. If the room spins, lie flat, raise the legs, and do not let the person “walk it off.”
Phase Three: Contextual Strategies — Reduce Noise Based on Where You Are
Environment can make a green-out much worse. Bright lights, too many voices, phone notifications, and public self-consciousness all increase the sense that something is going terribly wrong. Recovery often starts when stimulation drops.
1. Crowded Social Gatherings
Move out of the center of the room and into a quieter, dimmer space. Stay with one trusted person instead of a whole group. The goal is to stop the loop where embarrassment makes panic worse and panic makes the symptoms feel bigger.
2. Late Nights Alone
Use soft external anchors. Put on a familiar show, keep the room gently lit, and avoid doom-scrolling or searching worst-case symptoms. Sensory anchors such as lemon, mint, or the smell of black pepper can help pull attention back into the body, even if they are not proven antidotes.
3. Outdoors or Public Spaces
Sit down somewhere safe, cool the face or neck, and contact one steady person. Do not drive. Cannabis impairs reaction time, coordination, attention, and judgment, making driving dangerous and illegal.
Phase Four: Biochemical Interception — What May Help and What Is Overhyped
This is where emergency readers often get misled. There are plausible mechanisms behind some popular remedies, but plausible does not mean proven. In a green-out, they are secondary tools, not the main rescue plan.
1. Black Pepper and Lemon
Black pepper is popular because beta-caryophyllene has meaningful cannabinoid-related pharmacology, especially through CB2-linked signaling. But there is no strong human evidence that chewing peppercorns rapidly reverses THC intoxication. The better way to present it is as a grounding tool: a sharp smell or taste that interrupts panic and redirects attention.
2. CBD
CBD is often described as a rescue molecule because it can modulate CB1 signaling in laboratory settings. But human evidence does not justify presenting it as a dependable emergency fix. One controlled study found that some oral CBD doses did not reduce THC effects and that high-dose CBD could increase THC and 11-OH-THC exposure. In practical terms, if the person already knows CBD feels calming for them, it is optional. It is not the main protocol.
Phase Five: Somatic Anchoring and Metabolic Correction — Reclaim the Body
Once the first wave of panic drops, many users still feel unreal, detached, or physically unsteady. This is where body-boundary tools can help. A blanket, a couch corner, a pillow to hold, or a calm embrace can make the body feel more contained and less “out of body.”
If the person feels faint, address posture before assuming low blood sugar. Cannabis can contribute to lightheadedness and standing-related dizziness. A small bland snack is reasonable, but lying flat with the legs elevated often brings faster relief when the main problem is spinning or greying out on standing.
Summary: Build a Personal “Landing” Protocol
If someone wants to sober from weed fast because they are actively greening out, the highest-value advice is immediate grounding, not long-term detox talk. Stop consuming. Get somewhere quiet. Cool the face. Slow the exhale. Lie down if dizzy. Reduce noise and wait it out safely. New users need reassurance, edible users need patience, and older adults need fall prevention.
In 2026, the smartest landing protocol combines professional knowledge with better dose control habits. The physiology tools help in the moment. High-precision hardware helps lower the chance of getting there again. Download the Artrix Safe Consumption Whitepaper to explore device recommendations and safer-use strategies for different user profiles.
If a person becomes unresponsive but is still breathing, place them on their side while waiting for help. In the United States, Poison Help is available at 1-800-222-1222 for poisoning guidance.




















-1.webp)
-1.webp)
-2.webp)